TMD Management
A Historical Perspective
Temporomandibular disorder (TMD) comprises several co-occurring conditions that affect the anatomy and functionality of the temporomandibular joint (TMJ). The TMJ is the joint that connects the lower jaw (mandible) to the skull (temporal bone). TMD has been reported in between 3.7% and 12% of the population and is three to five times more frequent in women. The diagnosis, management, and prevention of TMD have been evolving in recent years. Here, we will present a brief overview of the history of TMD.

Multiple disciplines, multiple philosophies, multiple approaches, can leave patients feeling overwhelmed.
Twentieth Century
TMJ disorders started to be recognized by the medical community in the 1950s, but the symptoms were often dismissed as psychosomatic. It wasn’t until the 1980s that doctors, dentists, and healthcare scientists truly began to understand the causes of TMD and how to help suffering patients.
From 2000 to 2010
In the early 2000s, invasive treatments and surgical remedies for TMD came back into vogue, as there was also an increase in diagnoses. Invasive procedures such as arthrocentesis, which uses a syringe to collect fluid from a joint, were thought to be one of the best ways to make a diagnosis. However, by the end of the decade, studies proved that these procedures were unnecessary and in many cases, unhelpful.
From 2010 to Present Day
We understand much more about the mind-body connection than ever before, and the way behavioral interventions can help with some types of chronic pain, specifically TMD. Not only are these interventions less intensive and invasive from a medical side, but they are also more cost-effective for the healthcare industry as well as for the patient. Whether that is simply following patient self-care measures like the HEALS model—which teaches TMD sufferers best practices to alleviate current pain as well as prevent future flare-ups—or learning cognitive behavioral therapy skills (CBT), in many casaes, they are just as efficient if not more than other treatments used in the past.
Though the jury is still out on the long-term effectiveness of these treatments, it does seem that the prevalence of TMD is much higher among those who suffer from mental health problems such as anxiety and high stress. The psychological interventions for TMD may actually fix the issue, or they may just alleviate some of the pain and tension associated with it. But either way, it will help those who deal with TMD have a much more comfortable daily life, which is the ultimate goal.

Help for patients experiencing jaw pain is readily available!
Physiology of the Jaw
Jaw clenching, teeth grinding, and a misaligned bite are all signs of problems within the temporomandibular joint (TMJ), the one that connects your jaw to your skull. When one or all of those factors are in play, they can be detrimental to your quality of life. TMJ issues may lead to migraine headaches or pain whenever you talk or chew—hard things to ignore no matter your lifestyle. But what does that mean, really? If you suffer from TMJ disorder (TMD), learning about the physiology of the jaw could be a lifesaver, helping you remove unnecessary pain and discomfort from your everyday life.
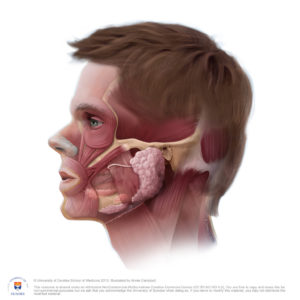
Features and Functions of the TMJ
Your TMJs are the most frequently used joints in the body—they are a necessity for basic survival functions, but they are the same things that are at risk of becoming a source of chronic pain. What makes the TMJ unique in our jaw physiology is the articular disk. This is a flexible piece of cartilage that serves as a cushion between the two bone surfaces of the mandible (jaw) and the temporal bone (bones on the lower lateral part of the skull, one on each side).
Because the cartilage lacks nerve endings or blood vessels, it is insensitive to pain. The front of the cartilage is attached to a muscle primarily responsible for chewing, and behind it is tissue that is full of blood vessels and nerve endings. Since the mandible is the only bone that moves while eating, knowing these facts about the anatomy of the jaw helps us to understand better why even a slight misalignment of the TMJ or its associated bones can cause so much pain. If the joint is out of place, every time we open our mouths, we are applying immense pressure on small and sensitive tissues that are close to our brain.

Left untreated, TMJ pain can lead to sensitization of the nervous system.
TMJ: Getting on Your Nerves
That small and sensitive tissue connects to a much more extensive neural network, which supplies nerves to most of the craniofacial region (the bones and muscles of the skull and face). Therefore, this affects more than just the mandible; this neural network is also connected to the ophthalmic system and even to the spinal cord. Even a millimeter or so can make a huge difference and bring pain throughout the entire body.
Unlike neural networks that are not directly connected to the craniofacial network, the TMJ area sends nerves to both the sympathetic and parasympathetic nervous systems. Effectively, this means that a similar injury or misalignment elsewhere in the body would only make for localized pain, but when concentrated in the TMJ, can send our nervous systems into total overdrive, and result in much more severe and debilitating pain.
The pain associated with TMD is deep, as well as diffuse. If each bite or yawn is painful, that will have a serious effect on the quality of life. As doctors, dentists, and scientists work together to learn more about these physiological systems and come up with solutions; there will be more hope of relief for those who suffer from TMD.
Diagnosis, Diagnosis, Diagnosis!
When suffering from Temporomandibular Joint (TMJ) pain or Temporomandibular Joint Disorder (TMD), getting a timely diagnosis and beginning pain management or treatment as soon as possible, is essential from both physical and psychological standpoints. Taking control of the pain and getting on the road to recovery requires a comprehensive diagnosis to ensure the correct pain relief and treatments are employed.
TMD can result from physical trauma, injury, jaw misalignment or a myriad of other physical conditions; it can also be psychosomatic.

Addressing acute injuries quickly minimize the risk of residual pain after trauma.
Improved Diagnostics
One of the first steps to diagnosis is to take a biomedical approach to the examination of the jaw. As methods of diagnosis have improved, and there is a greater understanding of how TMJ works, diagnosis of TMD has also been upgraded. This enhanced comprehension has had a massive impact on both clinical practice and research into treatment. Biomedical advancements have helped to create knowledge surrounding the classification of TMD subtypes, helping to develop standardization.
TMD medical specialists are better equipped than ever before to make a complete diagnosis and have a heightened awareness around both physical and psychological factors that may be impacting on the level of pain being reported by the sufferer. If psychosocial influences are not acting concurrently with the physical damage to the jaw, a purely biomedical approach to the resolution of the issue can be pursued.

Emotional and cognitive factors are important considerations for TMJ pain management.
Biomedical Model
Using a biomedical approach can initially define the subtype with further investigations, taking into account the emotional and cognitive factors necessary to create a rounded, holistic approach to the treatment and management of TMJ pain.
Other physiological factors, such as changes to the central nervous system that cause spasms or involuntary movements (hyperexcitation) or in how the brain’s neurons react to pain (neuroplastic changes) should be taken into account as possible causes of chronic pain.
By examining the visible and hidden physical causes of TMJ, doctors and dentists are in a better position to categorize the type of TMJ disorder the patient is suffering from and adjust treatments and pain management accordingly. If psychosocial influences are not acting concurrently with the physical damage to the jaw, a purely biomedical approach to the resolution of the issue can be pursued.
With a biomedical model for diagnosis used to ascertain the correct course of action, medical professionals can make recommendations for treatments such as oral appliances like dental splints, surgery or physiotherapy.

It is impossible to maintain a ‘good mood’ when suffering from acute TMJ pain.
Bio-Behavioural Approach to TMD Management
When you are suffering from acute pain such as that associated with Temporomandibular Joint Disorder (TMD), you would be forgiven for feeling emotional pain too. When pain is intense and causing significant discomfort, it is impossible to be in a good mood and firing on all cylinders.
TMD can be the result of, amongst other things, physical trauma, a facial injury, hormonal issues or jaw misalignment. Pain in the Temporomandibular Joint (TMJ), the joint connecting your jaw to your skull can be unrelenting and cause turmoil in your life if left untreated.

Diagnosis is the key to creating an effective treatment plan
Diagnosis Guides the Treatment Plan
After a diagnosis of TMD, you may feel upset or worried about how to resolve or manage the pain, and this is a normal reaction to learning you have a painful medical condition.
Your medical professionals will design a course of treatment to help alleviate the pain and to allow you to return to normal as quickly as possible. A thorough physical examination to determine the cause of the pain will be carried out so that an appropriate management plan can be put in place.
While the primary consideration of this treatment schedule will be focused on relieving the physical symptoms of TMD, medical professionals must take into account biobehavioral aspects of your care.
The biobehavioral approach scrutinizes the effects of the biological pain on your behavior—in other words, how your brain reacts to the physical pain you are going through.

How you think and feel about pain may have a direct influence on your healing experience.
Psychological Effects of Pain
Taking into account the psycho-social or how your thoughts and behaviors influence your experience and reaction to pain may help doctors to speed up your recovery or decide on different methods for managing it.
Your mood or state of mind can impact significantly on the levels of pain you are feeling and vice versa. By examining your psychological state, doctors can determine the best methods for managing your pain.
If you are suffering from depression or low mood, this may add to your perception of pain and increase the discomfort you are feeling. Your behaviors may even impact on the mobility of your jaw and prolong the treatment; it is vital for treatment to be comprehensive and take a holistic approach.
Your cognitive status may hinder your recovery, so taking a biobehavioral approach to treatment, in conjunction with biophysical methods, is necessary for a positive outcome to your treatment. There is little point in treating TMD with a dental splint worn at night if you spend your day clenching and grinding your teeth due to psycho-social factors causing you distress. To truly heal your TMD, other treatments to help lessen the psychological pain or behavioural issues you are experiencing must be introduced to relieve the stress on your jaw.
As you heal your physical pain, dealing with thought patterns and psychological issues should occur in tandem to help prevent recurring future flare-ups of TMD.
Residual pain is never easy to bear. It can disturb sleep patterns, making you more irritable and upsetting the balance of your mind. Taking a biobehavioral approach to pain management helps to detect the habits or behaviors that may be influencing the pain and help find a comprehensive remedy.

TMJ pain doesn’t have to take over your life! Small lifestyle changes have huge impact on pain reduction.
Biobehavioral Model of Pain Perception and Motor Behavior
Temporomandibular Joint (TMJ) pain or Temporomandibular disorders (TMD) can have an almost debilitating effect on your life. Suffering from any acute pain is a hindrance to quality of life and should be diagnosed and treated as soon as practicable. When this pain is coming from the joint attaching your jaw to your skull, it can cause additional issues as this joint is one that is in constant use.
Pain in the TMJ can cause issues when eating, talking, swallowing and even just relaxing; therefore, it impacts your day-to-day life. To ensure precise diagnosis, your medical professionals will physically examine your jaw for signs of damage to the TMJ and enquire about the nature of your pain. They may also take a biobehavioral approach to discover if psychological factors are impacting on your TMD.
How does a Biobehavioral Model help?
The biobehavioral model for diagnosing and treating TMD takes into account your emotional state, cognitive status, beliefs, behaviors and coping skills to ascertain how you will be able to manage your pain and resolve the issues in your TMJ. Studies have shown that your psychological well-being and state of mind can have a significant impact on your physical health, including the perception and management of pain.
Psychosocial factors are considered to be very significant in relation to chronic pain and its management, but it can also impact on motor behavior. The relationship between muscle and bone in the body can be fraught occasionally, causing musculoskeletal pain. This pain can result in changes in how you move or use your joints as you strive to avoid aggravating the injury.
When it comes to your TMJ, limiting movements are not always possible as you need to use the joint for so many activities. This means that to ease the strain on the joint or out of fear of inducing pain, you may get into the habit of holding your jaw differently or touching it a lot more than before.
Implementation of treatment and its likely outcomes are highly influenced by psychosocial factors. The perception and memory of pain, behavior in movement and willingness to undertake advised procedures will impact on how quickly TMD recovery occurs.
Therefore, using a biobehavioral approach offers a greater chance of relief from TMD due to the holistic manner in which a comprehensive diagnosis is achieved and how the issues are resolved.

Speed2Treat Home Healing Kit for Head, Neck or Jaw Pain, provides a 4-week guided self-care plan.
Management of Pain
Numerous methods are employed to manage the pain associated with TMD with the goal to ultimately curing the problem. These range from self-healing strategies such as using the HEALS method, dental splints or possibly surgery.
HEALS stands for:
Heat – applying a hot compress or an ice pack to the affected area
Exercise – moving and exercising the joint
Analgesics – treating the pain with OTC or prescribed medication
Lifestyle – implementing temporary or permanent changes regarding eating and sleeping habits
Stress/Strain – changing how you rest your jaw or put pressure on the joint
If you are experiencing delayed recover, even after utilizing the HEALS method, further intervention may be required. How you react to these treatments and your long-term prognosis is influenced by your behavior and state of mind. Your biobehavioral patterns may be the key to freeing your life from residual TMJ pain.
Multi-Modal Treatment Based on Biobehavioral Approach
When a Temporomandibular Disorder (TMD) has been diagnosed, pain management must be a key factor in the treatment plan. Living in constant pain can have lifelong impacts on somatic and psychosocial behaviors, and early treatment may prevent irreparable damage both to the joint itself and to your psychological reactions to pain.
The Temporomandibular Joint (TMJ) is the connection between your jaw and skull and is one of the most worked joints in the body. It is continuously used, even in sleep and is prone to injury. TMD can be the result of facial trauma, misalignment of teeth or jaw or numerous other factors including excess hormones in the early stages of pregnancy.
When a doctor or dental professional takes a biobehavioral approach to your TMD, they are trying to ensure that your treatment plan is wide-ranging and gets faster results. A biobehavioral model takes into consideration your frame of mind, perception of pain and cognitive status. By doing this, they are gauging how best to treat your TMD to optimize results.

Acute TMJ pain may be JAMSS – Jaw and Muscle Sprain or Strain
Benefits of Multi-Modal Treatments
Using a multi-modal treatment plan to address your pain issues may have longer-term effects on your physical and psychological health. This is due to the fact that by not just focusing on one aspect of treatment, the medical professionals–in consideration of psychosocial behaviors and physical elements–offer a more comprehensive environment for healing.
Your perception of pain, coupled with certain behaviors, impacts greatly on the methods of treatment suitable for your case. Those with a fear of pain or a high sensitivity to it, are more likely to struggle to complete prescribed exercises to free up the movement of the jaw. Therefore, doctors may have to find a more effective way to ease your TMJ pain.
The TMJ is a complex joint to heal as it is challenging to give it adequate rest if it is sprained or strained. The joint is active during talking, yawning, eating and resting, so a multi-modal approach is the only way to work towards pain resolution.

Reducing Stress and Strain in your life is a positive Lifestyle change that aids recovery.
Types of TMD Treatments
Using methods such as HEALS (Heat, Exercise, Analgesic, Lifestyle, Strain) to ease the pain may seem comprehensive as it includes manual or physiotherapy, pharmacology and soothing techniques. This method, however, is ineffective unless there is knowledge of the biobehavioral aspects of the patient. By having an understanding of your psychological state and the psychosocial influences that make you act as you do, doctors can formulate a treatment plan that is more likely to be successful.
Issues such as how you react to pain, how likely you are to follow routines or whether you get enough rest at night all feed into the structure of your treatment plan alongside the physical aspects of the TMD. Will you be able to bear the pain long enough to do the prescribed exercises? Do you sleep enough hours for a dental splint to be effective? Will stronger medications interfere with your brain’s chemical balance leaving you depressed or anxious? All of these factors must be considered.
This multi-modal approach is more likely to have a successful outcome than single-model methods of treatment as it takes a holistic approach to the problem, alleviating pain and returning the TMJ to normal function.

“Decrease your stress” is easy to say, not so easy to do. Cognitive Behavioral Therapy may help identify triggers.
Electrotherapy and Cognitive Behavioral Therapy for TMJ Pain
Patients and dentists alike are turning to less conventional forms of therapy to alleviate the pain associated with TMD. In this article, we will discuss electrotherapy in its various forms and Cognitive Behavioral Therapy, or CBT, and how they can help.
Electrotherapy
Electrotherapy, like the name implies, is the use of electrical currents to stimulate muscles and nerves after injury or strain. One of the most popular forms of electrotherapy for TMJ issues is the TENS unit. TENS stands for Transcutaneous Electrical Nerve Stimulation. The unit is a small machine with pads attached by a wire. The pads are somewhat sticky on one end, and are applied to the affected area.
The machine is then turned on, and power adjusted depending on the user’s preference and pain tolerance, and the machine effectively makes the muscles pulse in something like an auto-massage.
TMD is generally a result of pressure and strain of the nearby nerves and muscles. This causes something of a chain effect, pulling the surrounding muscles out of alignment as well, which then creates further pressure on other nerves — the TENS unit works to release this tension, thus actually targeting the mechanics of the problem as opposed to simply alleviating the associated pain. An added bonus is that TENS also causes the brain to release endorphins, which are hormones that, among its functions, acts as natural pain relief.
While some doctors will administer this treatment in their offices for 30 to 60 minutes at a time, because of their portable size and relative affordability, many choose to keep a unit at home to use for extended periods of time either regularly or to fight flare-ups.
Other electrotherapy options that have been proven to be helpful for TMD include short-wave diathermy, megapulse, ultrasound and soft laser. New electrotherapeutic technology is currently having something of a moment for TMD treatment, so is likely to become more common in the near future.
Cognitive Behavioral Therapy
The wear and tear of the temporomandibular joint that causes TMD is the clenching and grinding of the teeth and jaw muscles. As we have learned more about TMD in particular and stress-related chronic pain in general, more doctors are suggesting that their patients try CBT for long-term pain relief.
While many clinical psychologists and therapists are trained in CBT, and it is a popular treatment for afflictions such as anxiety and depression, a health psychologist will administer CBT if you are seeking it out specifically for TMD. The health psychologist will help you learn skills for pain relief, while also helping to diminish the stress that comes with having chronic pain. These skills will include things like progressive relaxation as well as more topics of conversation more traditionally associated with therapy, such as identifying and challenging negative thoughts, in the particular context of TMD. Studies have found CBT to be quite effective in helping TMD patients, especially when they are motivated and active participants in this less conventional form of treatment.
Managing your body’s responses to pain and stress on your own can make the whole ordeal feel even more painful and stressful. Trying therapies like electrotherapy or CBT can make the difference between suffering and relief, so talk to your doctor if you think it can help you.

Knowledge is Power! Arm yourself with education provided by experts in the field.
Education and Self Management Strategies/Relaxation
One of the major triggers for TMD is a ubiquitous problem in the modern world: stress. While we still live in society, certain aspects of stress will always be unavoidable. The ways in which we deal with them can be managed, and must be managed to keep TMD under control. Education is essential, both in terms of what the disorder actually is, as well as self-management and relaxation strategies that patients can bring into their daily lives.
Education and Self-Management Strategies
The most important thing to realize about TMD is that it is a systemic issue. Because the network of muscles, nerves and bones around the temporomandibular joint (TMJ), and the necessity of using them in everyday activities that we cannot avoid, like eating or talking, education is key for keeping excessive strain off the entire area.
HEALS – Self-Care Plan
An easy way to remember the lifestyle changes that help with TMD is a simple acronym: HEALS. HEALS is a list of the most important things to do to keep your TMD pain at bay.

Heat, Cold & Massage:
Applying ice and/or moist heat up to four times daily can help reduce pain and swelling.
Exercises:
Your doctor may recommend specific exercises for you to do on your own several times a day, which work to increase your jaw’s range of motion.
Analgesics:
Using over-the-counter pain relievers such as ibuprofen or acetaminophen not only helps to reduce pain, but the sooner they are taken, the more likely they will also help with jaw function.

An anterior deprogrammer, like the temporary QuickSplint, supports the TMJ to rest during sleep.
Lifestyle:
Making small, everyday choices can promote healing. This includes mindful chewing, using both sides of your mouth and opting for softer foods. Proper sleep hygiene is also crucial.
Stress/Strain Reduction:
Working on avoiding the habits and activities that stimulate TMJ pain is important to prevent symptoms from worsening. These include chewing gum, clenching or grinding your teeth, and resting your jaw on your hand.

Creating time to relax needs to be a lifelong habit…
And don’t forget to Relax…
Relaxation is easier said than done for many of us, but crucial for alleviating TMD pain — otherwise, you risk making it even worse!
A quick facial massage is helpful, and you don’t need to shell out hundreds of dollars to go to a spa to do it, either (though if you are able to do so, feel free!). A chiropractor or physical therapist can help, and there are medically approved exercises you can do at home to achieve similar effects. These exercises not only relax the muscles around the TMJ, but also work to strengthen and stretch them, which has long-lasting positive benefits.

Massage and mindfulness can be very helpful in recovering from head, neck or jaw pain.
Mindfulness comes into play here. Since TMD may be exacerbated by bruxism (teeth grinding and clenching) awareness of how our jaw is positioned throughout the day is a habit that needs to be broken. At first you may have to consciously think about it frequently, but it will become easier as you get into the habit.
Since small, repetitive habits combine to cause TMD, the best way to reverse it and prevent further pain and injury to the area is also going to be with small, repetitive habits.
Clinical Management of TMD
Temporomandibular disorder (TMD) is a group of neuromuscular and musculoskeletal conditions involving the temporomandibular joint (TMJ), the jawbone, and surrounding muscles. The TMJ sits in front of each ear and acts as a sliding hinge, connecting the lower jawbone to the skull. It is used in all jaw movement including when speaking, yawning, chewing, swallowing, and other such movements. Because the TMJ is frequently used throughout the day, disorders affecting it can be a painful experience. Common symptoms of TMD include jaw pain or dysfunction, earaches, headaches, and facial pain. Causes range from biological, emotional, cognitive, social, and environmental triggers.

Providers are standing by to help at www.facemypain.com
Diagnosis is usually based on history and physical examination. Many cases of TMD resolve themselves with or without a medical professional, and patients can reach for a range of noninvasive therapies, including self-care, physical therapy, patient education, cognitive behavioral therapy (CBT), and mouth guards. Chronic, consistent cases may benefit from prescription-strength relaxants, benzodiazepines, antidepressants, or injected pharmacotherapy. If these methods don’t help, a medical professional might suggest surgical intervention.
Various surgical interventions may be indicated.
Surgical Interventions:
Arthrocentesis
Arthrocentesis, or joint aspiration, is the minimally invasive procedure to remove chemical inflammatory mediators and reduce pressure that may cause stiffness or pain in the joint. The procedure consists of washing the TMJ and may include depositing a drug or other therapeutic substances. The recovery time for arthrocentesis is short, and the success rate is high. Studies have reported that this treatment has an average of 80% improvement in symptoms.
Arthrocentesis is usually the first form of surgical treatment in TMD cases because of its minimal invasiveness and high success rate.
Arthroscopy
Arthroscopy is a procedure that begins with opening a small hole in the skin above the joint. A narrow tube or cannula is then inserted through the hole and into the joint to create a safe and sterile way for the arthroscope and surgical tools.
An arthroscope is a tool with a camera and light that’s used to visualize the TMJ. Once it is in place with a stable image of the TMJ, the surgeon operates on the joint using small surgical tools also inserted through the cannula. With this surgery, the surgeon could also perform more complex procedures on the joint, including joint reshaping, scar tissue removal, and medical injection.
Arthroscopy is more invasive than arthrocentesis but less so than conventional open surgery. Recovery time is faster than open surgery, usually only lasting several days to a week.
Open-Joint Surgery
Open-joint TMJ surgery is an invasive procedure that begins with creating an incision a few inches long over the joint. The surgeon is then able to operate on the joint itself. This type of surgery is reserved for severe TMD, such as cases involving fusion of joint tissue, cartilage, or bone; tissue or bone growth that locks the joint into place; or cases with joints unable to be reached with arthroscopy.
In open-joint surgery, the surgeon can remove bony growths, excess tissues, and diseased bones. They are also able to reposition misaligned discs or replace discs damaged beyond repair.
While open surgery is invasive with longer recovery time, the success rate is reasonably high. Studies have found a 71% improvement in pain and 61% improvement in range of motion.
Recovery and Possible Complications
Most TMJ surgeries are outpatient procedures, meaning the patient can go home the same day as the surgery. Recovery times depend on the patient and the level of invasiveness of the performed procedure. NSAIDs are helpful for pain management, as is a change in diet to avoid any foods that might strain the joint. Cold compresses may help with any swelling.
The main and most common complication of TMJ surgery is the permanent loss in range of motion. Other possible complications include injury of facial nerves, infections around the surgical site, persistent pain, abnormal face swelling, and damage to nearby tissue.

Dental TMJ Specialists have a variety of tools available to alleviate acute or residual pain.
Dental Management
Engagement of the temporomandibular joint (TMJ) is impossible to avoid in everyday life. The TMJ is located in front of each ear and acts as the hinge that connects the lower jawbone to the skull. The joint is used when chewing, swallowing, speaking, yawning, and other such movements. Because it is used so frequently throughout the day, TMJ disorder (TMD) can be a painful experience ranging from mildly uncomfortable to unbearably excruciating. TMD symptoms include pain or tenderness in the jaw and surrounding jaw muscles, aching pain around the TMJ and ears, general facial pain, difficulty chewing, and locking of the jaw. Causes of TMJ disorders vary from external trauma, arthritis, misalignment of bite, or habitual grinding of teeth.
Many cases of TMD resolve themselves with or without the help of a medical professional, but it can cause many dental complications. When TMDs cause dental issues (or when dental issues cause TMDs), odontologists usually propose one of two approaches: orthopedic stabilization therapy and occlusal therapy. While TMD symptoms can’t be linked to specific types of malocclusion, TMD symptoms are often associated with malocclusion.
Orthopedic Stabilization Therapy
Splint therapy is the most commonly proposed conservative treatments for TMD pain associated with grinding of the teeth and misaligned bite. Splint therapy involves the use of plastic appliances which fit onto the teeth, affecting how the bite fits when the jaw joints are in varying positions. Palliative splints are used to relieve pain or improve debilitating conditions, while protective splints (such as mouthguards) are used to prevent teeth from wearing against each other. Occlusal splints, or orthotic devices, work best when specifically designed for the individual, especially concerning the treatment of TMD.
While the effectivity of TMD pain reduction through the use of stabilization splints has yet to be solidly determined, it appears that stabilization splint therapy may be beneficial for reducing pain severity at rest and on palpation and depression when compared to no treatment.
Occlusal Therapy
Occlusal therapy can include occlusal adjustment and/or orthodontic solutions.
Occlusal adjustments, or bite adjustment, is a procedure performed to remove small interferences that keep the teeth from coming together properly. Bite interferences, if not managed, prevent muscles of the jaw and neck from ever properly relaxing. This state can cause severe headaches, tooth pain, and neck aches—which may cause or be caused by TMD. Many patients may also grind their teeth, or begin grinding their teeth, as their jaw seeks its natural position. Teeth grinding can cause loss of tooth structure and receding gums. Occlusal adjustments are relatively simple: the doctor has the patient bite on a thin piece of paper which shows where the areas of contact occur. The doctor then smoothes these areas until the teeth meet together in a proper position.
Orthodontics is the branch of dentistry that corrects improperly positioned teeth and jaws. Some people who suffer from TMD seek orthodontic advice or solutions to realign their TMJ. While debates about the place of orthodontics as either cause or cure for TMD continues, some orthodontists have evolved their practices to specialize in treating TMJ disorders as well.

Dry Needling and Acupuncture
While up to 15% of adults may be affected by TMD, there is no definitive cure for the chronic problem. Surgery, orthodontics, and other aggressive treatments have not been proven to reduce the problem significantly, so many doctors, as well as patients, prefer to take a conservative approach. In recent times, some have turned to alternative therapies to supplement or replace traditional medicine. Dry needling and acupuncture have become particularly popular options for managing TMD pain.
Dry Needling and Acupuncture: Similarities and Differences
Acupuncture has been a common practice through Traditional Chinese Medicine (TCM) for approximately 3000 years. It has grown increasingly popular in the West in recent years, with over 10 million treatments administered each year in the United States alone. In the West it is commonly used to treat migraines, arthritis, and chronic pain, and has indications for many other physical and mental ailments. Acupuncture is performed by inserting long, thin needles into specific points of the body at various depths. Each acupuncture point is chosen to target different energy circuits or pathways (known as meridians) with the purpose of re-balancing energy (or “Qi”).
While dry needling looks similar in many ways, the reasoning behind the placement of the needles, as well as the aims of the procedure, are based in Western science. Dry needling is practiced by physical therapists with the goals of pain relief, improving range of motion, and/or addressing neuromuscular conditions. Dry needling has proven to reduce muscle tension and improve pain control.
Acupuncture and Dry Needling for TMD
For TMJ pain, dry needling will most likely involve placing needles directly at the source—your jaw, the joints and muscles surrounding it, and possibly even your neck or cervical spine, which plays a large part in the development of TMD. If you have a severe case of TMD, your physical therapist may even hook the needles up to an electrical stimulator which will get deeper into the tissue.
Studies have proven that acupuncture can be effective in reducing pain symptoms in TMD patients, and perhaps even as effective in reducing short-term pain symptoms as more conventional treatments. However, the methodology can be vastly different from that which is used in dry needling—they are balancing the Qi in the liver meridian, which has a deficiency, and the gallbladder meridian, which has an excess. Because of this, while the acupuncturist may insert needles into the jaw and surrounding area, they may also insert needles in the areas around the elbows, knees, and big toe.
Admittedly, there is significant overlap in both treatments, so in many ways, it is an apples-to-apples comparison. Both are relatively safe, rely on needles, and have proven efficacy in pain relief both generally as well as specifically TMD related pain. Acupuncture has the wisdom of the ages on its side, but for those who feel safer with more medicalized and evidence-based treatments, dry needling may be preferable.

Manual Therapy/Therapeutic Exercise
TMD can be an overwhelming diagnosis to receive with many different factors to consider. While it is not an easy fix, there are many inexpensive and noninvasive ways to manage the general pain and discomfort of TMD—and some can even be practiced from the comfort of your own home, after learning the proper protocols.
Most doctors take a conservative approach to dealing with TMD, which usually results in clinically satisfactory outcomes for mild-to-moderate cases.
Therapeutic Exercise After TMJ Injury: Speed2Treat Protocol
If you have recently experienced jaw and muscle strain or sprain (often referred to as JAMSS) you can take preventative measures in the days and weeks after the injury to save you significant suffering in the long term. The first 30 days after injury are the most critical to begin treatment; if the strain or sprain is not resolved within that window, the jaw joints and muscles may have a greater than 50% chance of progressing to chronic pain.
Unlike a strain or sprain in another part of the body, the jaw cannot be rested and given time to heal on its own because it is a necessary component for daily life. This is why treatment protocols such as the Speed-to-Treat Protocol can be such a game-changer if introduced early enough. The protocol is a comprehensive plan to evaluate and manage acute sprain or strain in those crucial early days.

Self-Care is a key component in your recovery.
HEALS and Jaw Rx-Ercises: Patient Self-Care Measures
Some of the most important measures a patient with TMD or JAMSS can take are methods that they can do anytime, anywhere. These are the core components of the recovery process.
HEALS is an acronym that outlines the five things your TMJ and jaw muscles need.
H stands for heat, cold and massage. Applying heat or ice up to four times a day can help with pain by reducing swelling and relaxing the muscles. Since swelling is likely to be worst directly after an injury, cold is used most frequently in the first 24 hours, but whatever is most comfortable for the patient is always the best option.
E stands for exercises, which gradually helps extend the range of motion in your jaw. The Jaw Rx-ercises are specially designed to help train your body to subconsciously keep your jaw and tongue in the proper position to avoid clenching. At first, they should be practiced throughout the day—up to 30 times a day—to help commit the actions to muscle memory.
A stands for analgesics, such as ibuprofen or acetaminophen. Taking an over-the-counter anti-inflammatory and pain-reducing medication is helpful to control pain, which will ultimately benefit overall jaw function.
L stands for lifestyle. TMD can have a severe effect on your life; making positive lifestyle choices will help promote and speed up healing. The food you choose to eat, the activities you partake in, and the amount of rest you prioritize are all important in controlling these painful problems.
S stands for stress or strain. Reducing habits that cause muscles to tense, and avoiding activities that strain the jaw, will make a world of difference in terms of pain. Continuing the jaw exercises regularly and avoiding problematic behaviors are the difference between chronic pain and a happy jaw.
While your jaw pain may not be cured completely, these easy steps to follow in your daily life can influence whether you become a chronic TMD sufferer or not.
FaceMyPain opens a path to care with qualified doctors and other healthcare providers who understand the complexities of facial pain and can help you find relief and healing.
Treatment providers featured in the FaceMyPain directory are orofacial pain specialists, neurologists, osteopaths, dentists, oral surgeons, physical therapists, chiropractors, and other providers dedicated to treating facial pain conditions.





